

Endoscopic Retrograde Cholangiopancreatography (ERCP)
Back to topWhat is the purpose of this procedure?
The main goal of ERCP is to treat problems in the bile and pancreatic ducts using a thin, flexible tube called an endoscope. To determine if you would benefit from this procedure, doctors would do noninvasive tests first such as computed tomography, magnetic resonance cholangiopancreatography, or endoscopic ultrasound. These tests are less risky than ERCP and diagnose problems of the bile duct and pancreatic duct. In patients with chronic pancreatitis, the purpose of an ERCP is usually to remove a pancreatic duct stone or to open a blocked pancreatic duct or bile duct.
What happens during the ERCP procedure?
Before the procedure, you will be given a sedative or medicine to help you stay relaxed and comfortable during the procedure. You may or may not be awake, but either way, you probably won’t remember any of it. A health care professional will place an intravenous (IV) needle in your arm or hand to give you the sedative.
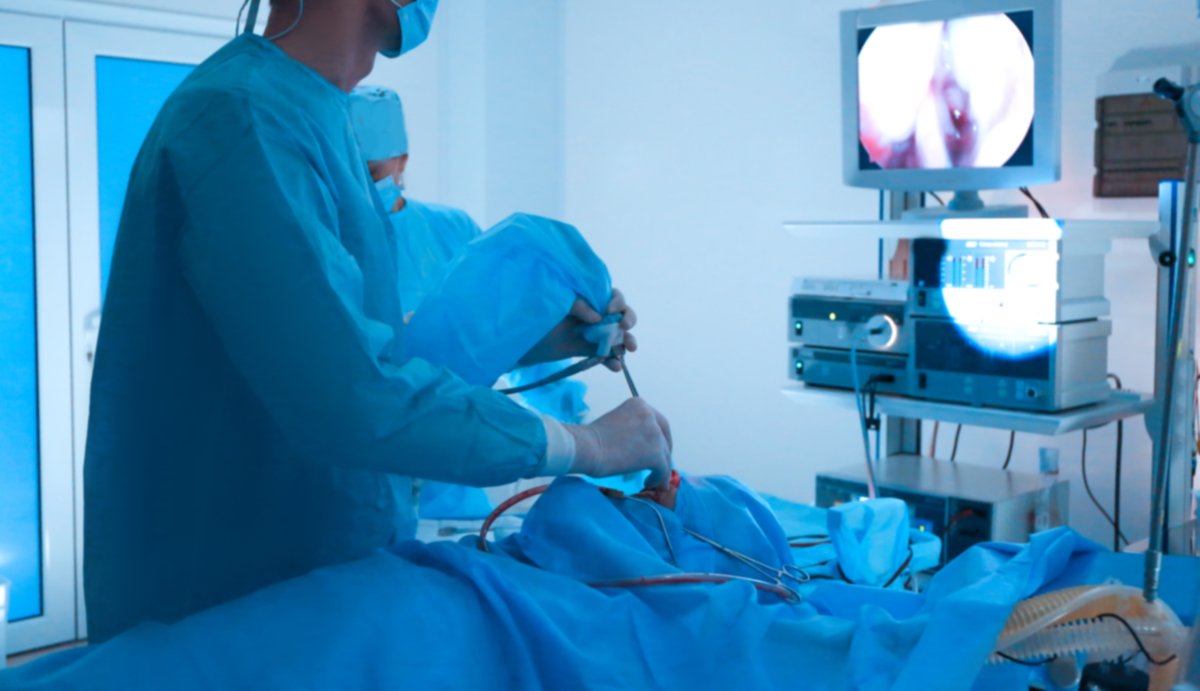
You’ll be asked to lie on an exam table. When you are ready, the doctor will carefully pass the endoscope down your esophagus and into your stomach and duodenum. The endoscope pumps air into your stomach and duodenum, making them easier to see. A small camera mounted on the endoscope will send a video image to a monitor.
During ERCP, the doctor locates where the bile and pancreatic ducts empty into the duodenum. The doctor will then slide a thin, flexible tube called a catheter through the endoscope and into the bile and pancreatic ducts. The doctor injects a special dye through the catheter into the ducts. The dye will make the ducts more visible on x-rays. The doctor uses a type of x-ray imaging, called fluoroscopy, to examine the ducts and look for narrowed areas or blockages. The doctor may pass tiny tools through the endoscope to treat problems in the bile and pancreatic ducts.
The procedure takes about 90 minutes, but expect your visit to last 3 to 4 hours to allow for preparation, follow-up with the doctor, and recovery.
What interventions are done for chronic pancreatitis during ERCP?
Depending on the findings, the doctor may perform one or more of the following interventions during the ERCP procedure:
- Sphincterotomy: If needed, the doctor may cut the muscle (sphincter) at the opening of the bile or pancreatic duct to help improve drainage or allow for easier removal of stones. This is often done during your first ERCP procedure and facilitates the entry to the duct in subsequent procedures.
- Stone removal: If gallstones or pancreatic stones are blocking the ducts, the gastroenterologist may use special tools such as balloons or baskets to extract the stones.
- Lithotripsy: This refers to breaking stones into small pieces. Larger or harder stones sometimes need to be broken into smaller pieces before they can be removed. Lithotripsy can be performed internally during ERCP using specialized tools passed through the endoscope. In some cases, lithotripsy may be performed externally using focused sound waves in a procedure called Extracorporeal Shock Wave Lithotripsy (ESWL). This method is non-invasive and is typically used when internal methods are not feasible. Sometimes ESWL is performed by a urology specialist.
- Stent placement: If a biliary or pancreatic duct is narrowed or blocked, a small plastic or metal tube (stent) can be placed to hold it open and slowly open up the narrowing. This allows bile or pancreatic fluid to drain properly and relieve your symptoms.
- Balloon dilation: This involves dilating or stretching a narrowed duct with an inflated balloon to widen the duct.
- Biopsy: In some cases, small tissue samples may be collected for further testing if there is a concern about cancer or other diseases.
Who performs an ERCP?
Not every gastroenterologist performs ERCPs. Some gastroenterologists undergo special training to learn performing this procedure and are called interventional endoscopists or advanced endoscopists. Rarely non-gastroenterologists as surgeons may perform ERCPs. It is important to have a doctor who has training and skills in treating pancreatic problems. Not every provider performing ERCPs has experience treating chronic pancreatitis. Large referral centers will often have more expertise performing ERCPs in patients with chronic pancreatitis.
What are the risks associated with this procedure?
The risks of ERCP include:
- Acute pancreatitis. This is the most frequent complication of ERCP. This refers to acute inflammation of the pancreas causing severe abdominal pain. This is temporal but often needs a hospital admission post procedure to monitor your symptoms and to provide you treatment with fluids and pain medications. The risk of post ERCP pancreatitis is variable depending on the procedure indication and complexity of your ERCP. The risk can range from 5% to 15%. To reduce your risk of acute pancreatitis, your doctor may give you a suppository medication (e.g. indomethacin) during your procedure, which has demonstrated to reduce the risk of acute pancreatitis. The risk of pancreatitis is also reduced by giving intravenous fluids and putting pancreatic stents.
- Bleeding. This happens rarely in 1% of procedures and is more common when the opening of the duct is cut (sphincterotomy). The bleeding is usually small and stops on its own. However, sometimes the bleeding can be more severe. When bleeding is more severe, this can be treated endoscopically with metal clips, injection of epinephrine, burning the area with electricity, or putting stents. If the bleeding does not improve by this method, patients may need a radiologic procedure. Sometimes patients may need blood transfusions if the bleeding is too severe.
- Perforation. This refers to a tear in the intestines or biliary ducts. This happens in less than 1% of procedures. If this is small, it may heal on its own with closely watching you in the hospital. If it’s big, then it may need endoscopy or surgery to fix it.
- Infection of the bile ducts (cholangitis). This rarely happens and is treated with antibiotics when present. Fevers and abdominal pain may be a sign of infection.
- Allergic reaction to sedation or contrast dye
Is ERCP a major surgery?
ERCP is not considered major surgery. Unlike traditional surgery, which often involves cutting through the skin to access internal organs, ERCP is performed with an endoscope—a flexible tube inserted through your mouth and guided into your digestive system. This allows your doctor to examine your bile ducts and pancreas using X-rays, without making any external cuts. During ERCP, your doctor can pass special tools through the endoscope to perform small treatments inside your body. While these are sometimes called “endoscopic surgeries,” they are minor compared to traditional surgery, with fewer risks, less pain, and quicker recovery.
How should I prepare for the procedure?
You must have a driver with you at the time of check-in and check-out. Your driver must accompany you for your procedure. You can be discharged only to the care of a responsible adult driver 18 years of age or older because sedatives will make you drowsy.
- Since you will be receiving sedation, it is important that you do not eat within 8 hours before the procedure. Small amounts of clear liquids are ok up to 2 hours before the procedure. If you have diabetes, discuss an eating and medication schedule with your doctor.
- You may need to stop taking certain medications several days before the procedure. Please remind the doctor’s team of all prescriptions, especially diabetes medications and blood thinners. The doctor will tell you if and when you need to discontinue the medications.
- Tell the doctor if you develop a cold, fever, or flu symptoms before your scheduled appointment, or if you have started taking antibiotics for an infection.
What happens after the procedure?
After the procedure you will be taken to the recovery area where you will spend about 60 minutes. You may feel bloated or have a sore throat for a day. Some mild abdominal discomfort is common, but seek immediate care if you have severe pain, fever, blood in your stool, black stools, chest pain, trouble swallowing or vomiting, which may indicate a complication like pancreatitis.
To achieve successful treatment of pancreatic duct blockades or stones, several ERCP procedures are needed. On average, patients need between 3 to 5 ERCP procedures over the span of 6 to 12 months.
You can watch the following video to learn more details about ERCPs:
Extracorporeal Shock Wave Lithotripsy (ESWL)
Back to topWhat is the purpose of this procedure?
ESWL is a procedure that consists of short-duration, high-energy shockwaves that are produced outside the body by a lithotripter. This procedure doesn't require surgery and is commonly performed to break kidney stones and is also used to break up stones in the pancreatic duct . The goal is to fragment large or hard stones into smaller pieces so they can spontaneously pass through the ducts or be more easily removed during ERCP. ESWL is commonly used in chronic pancreatitis when stones are causing ductal obstruction and pain.
What happens during an ESWL procedure?
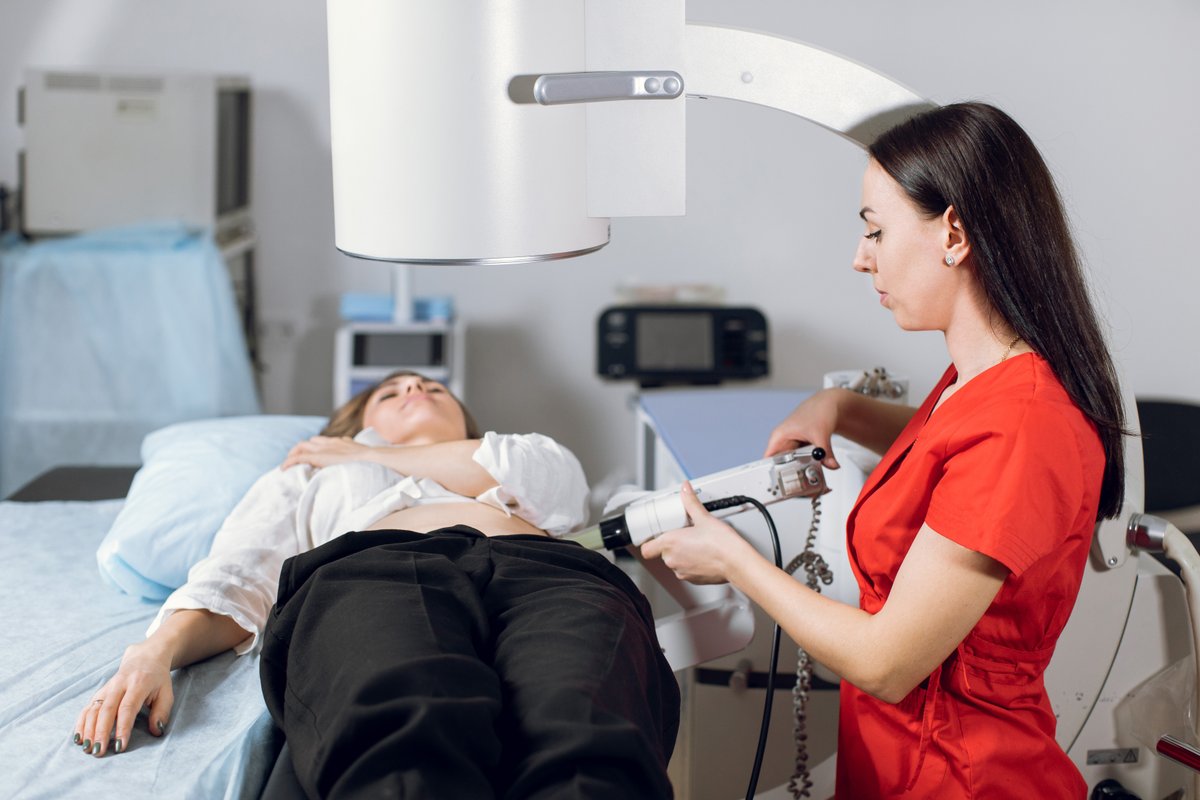
X-rays will be obtained during the procedure. You may receive an antibiotic, either by mouth or through an IV, right before the procedure. The anesthesia team will attach monitoring devices to you. Generally speaking, your procedure can be done with just intravenous sedation; however, in a small number of cases general anesthesia is required. Most of the time, you will lie on your back for the procedure. Depending on your stone's location, you may lie on your stomach on the procedure table.
The focus of the lithotripter is positioned on the stone using X-ray or ultrasound imaging. The shockwave generator is then pressed against your side. A cold gel is applied in between the shockwave generator and your skin.
Your procedure will take 30 to 60 minutes to complete. Treatment time is dependent on your stone's size and hardness. Progress is assessed in real time with X-ray and/or ultrasound imaging. It is important for you to remain still during treatment to keep your stone in focus.
Who performs an ESWL procedure?
This is performed by urologists or gastroenterologists with training on performing ESWL. This may occur in the operating room, endoscopy suite, or outpatient procedure center that has the lithotripser equipment to perform these procedures.
What are the risks associated with this procedure?
The risks are infrequent. They include:
- Abdominal pain or discomfort during or after the procedure
- Mild bruising or soreness at the site where shock waves are applied
- Incomplete stone fragmentation, which may require repeat sessions
- Pancreatitis or inflammation of nearby tissues
- Nausea or vomiting
- Rarely, bleeding or infection
What should I expect after the procedure?
After the procedure, there is a short observation period. You are able to return home after this brief period. After the procedure, you may feel sore or bruised in the upper abdomen or back for a day or two. It's important to drink plenty of fluids to help flush out the stone fragments, which may pass in your stool. Contact your doctor if you develop fever, severe pain, vomiting, or signs of infection.
If the stone is not completely pulverized, you may need additional ESWL and ERCP procedures to completely clear your pancreatic duct.
Endoscopic Ultrasound (EUS)
Back to topWhat is the purpose of this procedure?
Endoscopic ultrasound, also known as EUS, is both a treatment tool and a diagnostic tool. This consists of a flexible tube with a small ultrasound probe at its tip to examine the lining and walls of the gastrointestinal tract and the surrounding internal organs such as the pancreas, bile duct, and gallbladder. In addition, EUS can be used to drain fluid collections, perform nerve blocks, and to create connections with the stomach or intestine with normal organs (e.g. bile duct, pancreas, jejunum).
What happens during an EUS procedure?
Before beginning the procedure, you will have an intravenous (IV) line started to give you a sedative. You will lie on your left side while connected to oxygen and blood pressure monitors. The sedative will make you comfortable and sleepy.
If the goal is to examine the pancreas and surrounding peripancreatic areas, the doctor will pass the endoscope through your mouth and into your digestive tract. The ultrasound component produces sound waves that create detailed, visual images of the digestive tract.
The procedure takes between 15-45 minutes. However, you should plan for your entire visit to last about 2 to 3 hours, which includes preparation time, follow-up with the doctor, and recovery.
What interventions are done for chronic pancreatitis during EUS?
Depending on the findings, the doctor may perform one or more of the following interventions during the EUS procedure:
- Biopsy: EUS is often used to guide a thin needle to suspicious areas (e.g., tumors, cysts or lymph nodes) to collect tissue or fluid samples for further analysis. If a sample is obtained, the results will usually take a few days until they are finalized. Tell your doctor about what's your preferred method to receive results.
- Drainage of fluid collections: In cases of symptomatic pancreatic fluid collections, EUS can be used to guide the placement of stents or drainage catheters through the stomach or duodenum wall to safely drain the fluid. If a stent is placed, it is usually temporary and will be removed after a few weeks, as indicated by your doctor.
- Celiac plexus block: If you suffer from severe abdominal pain related to chronic pancreatitis, a celiac plexus block may be performed. This involves injecting a numbing medication around a group of nerves (the celiac plexus) to relieve pain. More details about this procedure are provided in a later section.
Who performs an EUS?
An EUS is typically performed by a gastroenterologist who has received specialized training in advanced endoscopic procedures. It is important that the doctor performing your EUS has the appropriate expertise and experience in diagnosing and treating pancreatic conditions.
What are the risks associated with this procedure?
The risks vary depending on the type of intervention performed during your EUS. While complications are uncommon, they may include:
- Sore throat or discomfort after the procedure.
- Bleeding, especially if a biopsy or drainage is performed.
- Perforation (tear) in the digestive tract.
- Acute pancreatitis or inflammation of your pancreas, causing severe pain.
- Infection.
- Allergic reaction to sedation or injected substances.
How should I prepare for the procedure?
Preparation is similar to ERCP preparation.
What should I expect after the procedure?
After the procedure, you will be taken to a recovery room where your driver can join you and you will receive discharge instructions. The doctor who performed the procedure will explain the preliminary results to you and give the complete results to the doctor who ordered your procedure. Some mild abdominal discomfort is common, but seek immediate care if you have severe pain, fever, or vomiting.
You can watch the following video to learn more details about EUS.
Celiac plexus block (CPB)
Back to topWhat is the purpose of this procedure?
CPB is a procedure used to reduce chronic abdominal pain, often performed in patients with chronic pancreatitis. CPB works by injecting medications that temporarily block nerve signals (block) or destroys nerves (neurolysis) around the celiac plexus. The celiac plexus is an area in front of the spine. This area has a group of nerves that transport pain sensations from the internal organs located in the upper abdomen (stomach area). These organs include the pancreas, liver, gall bladder, small bowel and part of the large bowel. A local anesthetic and/or steroid medications are often used to numb these nerves. Alcohol can sometimes be used to destroy the nerves, especially for pancreatic cancer. This stops the nerves from feeling pain.
How is the CPB performed?
CPB can be performed using several approaches, depending on your anatomy, medical condition, and the physician's expertise. All techniques involve guiding a needle to the area around the celiac plexus using imaging for accuracy and safety. The procedure may be done through the skin or by endoscopy:
- Percutaneous approach: a needle is inserted through the skin in the back or front of the abdomen, and advanced toward the celiac plexus under Xray guidance.
- Endoscopic ultrasound-guided (EUS) approach: an endoscope with an ultrasound is passed through the mouth into the stomach. A fine needle is then inserted through the stomach wall under direct ultrasound guidance to reach the celiac plexus.
What are the risks associated with this procedure?
The risks are infrequent. They include:
- Low blood pressure, especially when standing up: this is temporal and resolves in hours or days.
- Diarrhea: this is temporal and resolves in days.
- Infection.
- No improvement or worsening abdominal pain.
- Bleeding or hematoma.
- Organ injury (e.g., liver, stomach, kidneys) (rare).
- Spinal cord injury or paralysis (very rare).
What should I expect after the procedure?
After the procedure you will be taken to the recovery area where you will spend about 60 minutes. You may feel mild back pain or abdominal discomfort for a day or two. Some people experience temporary low blood pressure or diarrhea due to the nerve block's effects. Contact your doctor if you experience severe pain, fever, leg weakness, or signs of infection.
About half of the patients feel some or total relief from pain after the procedure. Since the nerve block typically lasts three to six months, patients may need to repeat the procedure if there is improvement.
Pancreatic surgery
Back to topWhat is the purpose of pancreatic surgery?
Pancreatic surgery in patients with chronic pancreatitis is primarily performed to relieve persistent, severe pain that does not respond to other therapies. Surgery can also help manage complications such as bile duct or duodenal obstruction, or the presence of pancreatic fluid collections. The types of surgical procedures may include drainage, resection, or a combination of both, depending on the disease's location and severity. Ultimately, the goal of surgery is improving quality of life and preventing further complications.
What are indications for pancreatic surgery in chronic pancreatitis?
Surgery in chronic pancreatitis is recommended for the following indications:
- Severe abdominal pain unresponsive to other therapies
- Complications such as biliary or duodenal obstruction
- Suspected or confirmed pancreatic cancer or neoplastic lesions
- Recurrent or persistent symptomatic fluid collection
- Local vascular complications (e.g. bleeding, portal vein thrombosis)
When is a good time to consider pancreatic surgery in chronic pancreatitis?
Research shows that early surgery for chronic pancreatitis can offer significant benefits, such as better pain control, preservation of pancreatic function, and improved quality of life compared to delayed surgery. For this reason, it's important to discuss the timing, risks, and benefits of surgery with your doctor early in your treatment journey. Together, you can decide on the approach that's best for you. In many cases, you and your doctor will try less invasive treatments first—such as medications or endoscopic therapy—and reserve surgery for situations where these options do not provide enough relief.
Who performs pancreatic surgery?
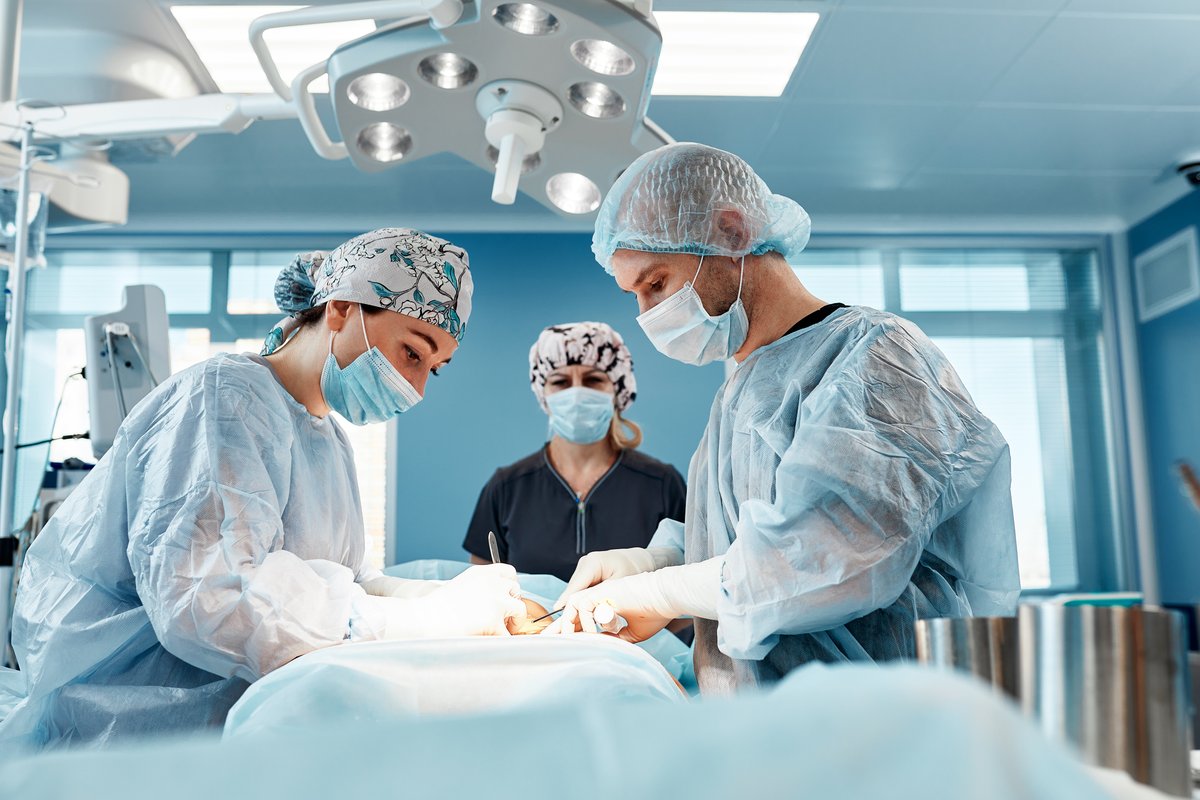
Pancreatic surgery is performed by trained surgeons who specialize in pancreas and hepatobiliary surgery. These procedures should be done in high-volume referral centers with experience in managing complex pancreatic diseases. Surgery is usually coordinated as part of a multidisciplinary team.
What are the options for chronic pancreatitis surgery?
The type of pancreatic surgery depends on the disease and the part of the pancreas affected. The most common procedures include:
- Whipple's Procedure (Pancreaticoduodenectomy): Removes the head of the pancreas, part of the small intestine (duodenum), gallbladder, and sometimes part of the stomach.
- Distal Pancreatectomy: Removes the most distal part of the pancreas, called the body and tail of the pancreas. Sometimes the spleen is also removed.
- Puestow Procedure (Longitudinal Pancreaticojejunostomy): In this procedure, the surgeon opens the length of the main pancreatic duct and connects it directly to the small intestine. This new connection allows better drainage of pancreatic fluids, which can help relieve pain and reduce symptoms by decreasing pressure inside the pancreas.
- Beger Procedure: Removes the inflamed head of the pancreas while preserving as much healthy pancreatic tissue and nearby structures as possible.
- Frey Operation: combines removal of tissue from the head of the pancreas with a connection between the pancreatic duct and the small intestine to improve drainage.
- Total Pancreatectomy: Removes the entire pancreas, gallbladder, part of the stomach, and sometimes the spleen. Patients will need lifelong insulin and enzyme replacement.
- Total Pancreatectomy with Islet Autotransplantation: the entire pancreas is removed, and the insulin-producing islet cells are isolated from the pancreas and then infused into the patient's liver. If the islet cells survive, they can continue to produce insulin, reducing or eliminating the need for insulin. This will be discussed in more detail in a different section. -
What are the risks associated with pancreatic surgery?
Pancreatic surgery is a complex procedure and involves important nearby structures. While many patients recover well, there are potential risks, including:
- Bleeding during or after surgery
- Infection (wound or internal)
- Leakage of pancreatic or digestive fluids
- Delayed gastric emptying (slow stomach function)
- Diabetes (if much of the pancreas is removed)
- Digestive difficulties or malabsorption
- Blood clots or lung complications
- Reoperation in some cases
What happens after the surgery?
- Most patients stay in the hospital for 5–10 days depending on the procedure and recovery.
- You'll receive pain control through IV or epidural medications, gradually transitioning to oral medications.
- You may start with oral fluids and gradually progress to soft foods.
- Enzyme supplements may be prescribed if digestion is affected.
- Your surgeon will monitor healing, blood sugar levels, and nutritional status. Long-term follow-up may include imaging, blood tests, and endocrinology or gastroenterology care.
Total Pancreatectomy with Islet Autotransplantation (TPIAT)
Back to topWhat is the purpose of this procedure?
TPIAT is a surgical option for patients with debilitating chronic or recurrent pancreatitis whose symptoms have not improved with other methods. The primary goal of the procedure is to relieve abdominal pain and improve quality of life, while attempting to preserve insulin production by transplanting the patient's own islet cells. Unlike other transplant procedures, TPIAT does not require immunosuppressive drugs because the islets come from the patient's own body.
What happens during the TPIAT procedure?
TPIAT consists of two main parts:
- Total Pancreatectomy (TP): The entire pancreas is surgically removed. In most cases, the spleen and part of the small intestine (duodenum) are also removed.
- Islet Autotransplantation (IAT): While the surgery is being performed, a specialized laboratory team processes the removed pancreas to isolate insulin-producing islet cells. The islets are then infused into the liver, where they may begin producing insulin over time.
The entire operation may take 7 to 10 hours.
Who is a candidate for TPIAT?
Every center has different requirements. Overall, this surgery is considered for patients with chronic or recurrent acute pancreatitis who have:
- Pain that is severe enough to cause disability (missing school, work, family life, etc.) and/or results in opioid dependence
- Little or no existing diabetes and still have healthy islet cells in the pancreas
- Any other physical and mental health issues adequately managed and under control
- Completely stopped smoking before and after the surgery, if they are smokers
- Commitment to a long and difficult recovery
- Commitment to lifelong pancreatic enzymes, monitoring complications, and likely diabetes
- Completed a thorough evaluation by a multidisciplinary medical team who recommended this procedure
Who performs TPIAT?
Only a few surgeons and centers perform TPIAT. For a list of centers that perform this procedure, you can visit Mission:Cure website
What are the risks of the procedure?
TPIAT is a major surgery with several risks, including:
- Surgical complications such as bleeding, infection, or bowel leaks.
- The chance that the transplanted islets may not work well or may stop working.
- Prolonged hospital stays or need for reoperation.
- Fat malabsorption and nutritional deficiencies, requiring lifelong pancreatic enzymes and vitamin supplementation.
- About 1 in 4 patients still have daily abdominal pain and need pain medication a year after surgery, so pain relief is not guaranteed for everyone. This may be due to pain originating in the nervous system and not directly from the pancreas.
- More than half of the patients will have diabetes and will need to take insulin long-term to manage the blood sugars. This is influenced by the number of islets that the pancreas had and that are successfully transplanted.
What happens after the TPIAT?
After surgery, patients typically stay in the hospital for 1–2 weeks. However, the recovery time can last for about 1 year. All patients will have temporary diabetes and need insulin at first. During this recovery phase, the treatment team will try to wean off the pain medications, wean off the insulin if possible, transition to a regular diet, adjust the pancreatic enzymes, and monitor laboratory tests. Most people experience significant improvement in pain after surgery, and quality of life often improves, with many patients returning to work, school, and daily activities.
Enteral feeding
Back to topWhat is enteral feeding?
Enteral feeding is a method of providing nutrition through a tube placed into the stomach or small intestine. This approach is used when patients are not meeting their nutritional needs or to rest the pancreas to decrease pain. Enteral feeding can help prevent malnutrition, support healing, and reduce the workload on the pancreas by bypassing normal digestion. It is often recommended during hospitalizations, periods of severe symptoms, or in cases of long-term poor intake, and is considered a safer and more effective option than intravenous nutrition when the digestive tract is still working.
What are options for enteral feeding?
Enteral feeding options depend on how long support is needed and where the nutrients should go in the digestive system. Here are the main types: Short-term options (days to weeks)
- Nasogastric tube: inserted through the nose into the stomach. Used for short-term support, especially during flares or hospital stays
- Nasojejunal or nasoduodenal tube: inserted through the nose into the small intestine. This can be removed at any time if it's causing you too much discomfort
Long-term options (weeks to months or more)
- Gastrostomy (G-tube): placed through the skin directly into the stomach
- Gastrojejunostomy (GJ-tube): allows feeding into the jejunum through a stomach port
- Jejunostomy (J-tube): placed through the skin directly into the jejunum, allowing it to feed directly into the small intestine
What will I receive through the feeding tube?
You will receive a liquid formula that includes all the nutrients your body needs, such as protein, vitamins, minerals, fluids, and water. There are different types of formulas:
- Standard formulas are used for most people and contain a mix of carbohydrates, protein, and fat
- Specialized formulas may be used if you have other conditions such as kidney disease, problems absorbing nutrients, or need fluid restriction
In addition to formula, water is given through the feeding tube to keep you hydrated and to flush the tube, preventing it from clogging. Sometimes, medications can also be given through the feeding tube if they are in liquid form. For tubes in the nose, crushed and dissolved tablets should be avoided as they can clog the tube.
Who manages my enteral feeding?
Your healthcare team will work together to manage your feeding plan, whether you are in the hospital or at home:
- Physician: Oversees your overall care and makes decisions about tube placement and feeding needs
- Dietitian: Chooses the right formula and ensure you're getting the correct amount of calories, protein, and fluids
- Nurse: Manages the feeding process and teaches you and your caregivers how to safely use and care for the tube at home
When you are in the hospital, the medical team will monitor your tolerance to the feeding, check your labs daily, and adjust your plan as needed. Once you are home, you or a caregiver will handle the formula preparation, administer the feedings, and manage the tube. You'll also have follow-up visits to review your progress and make any needed changes to your nutrition plan.
How do I care for my feeding tube at home?
Taking good care of your feeding tube helps prevent problems like infections, blockages, or leaks. Here are some tips:
Flush the tube regularly: Use clean water to flush the tube before and after each feeding and medication. This keeps the tube from clogging. Your care team will tell you how much water to use and how often.
Do not put anything in the tube unless instructed: Only use formula, water, or medications approved by your care team. Never put soda, juice, or crushed pills without checking first. They can clog or damage the tube.
Follow your schedule: Stick to the feeding plan and schedule given by your healthcare team. Let them know if you're having trouble finishing feeds or feel unwell.
Keep the site clean and dry (if placed through your skin): Clean the skin around the tube daily with mild soap and water. Dry the area gently and check for signs of redness, swelling, or discharge.
Secure the tube (if placed in the nose): keep the tube holder or tape that was placed to prevent the tube pulling out of place. If a tape was placed, change it periodically.
Your care team will show you exactly how to do all of this before you leave the hospital and will provide written instructions for you and your caregivers.
What are the possible complications of enteral feeding?
Enteral feeding is generally safe and well tolerated, but the following complications can occur:
- Feeding intolerance: Some people may feel bloated, nauseated, or have diarrhea or abdominal discomfort when starting feeds
- Aspiration: This happens when formula accidentally enters the lungs. Keeping the head of the bed elevated when you are receiving feedings helps reduce this risk
- Infections: The site where the feeding tube enters the body (such as the skin of your abdomen) can become red, painful, or infected—especially with long-term tubes. If you notice fever or any of these signs, contact your healthcare provider
- Tube problems: The tube can get blocked, move out of place, or leak. Regular flushing with water helps prevent clogging
- Constipation or diarrhea: These are common and may be related to the formula, medications, or reduced movement
- Electrolyte imbalances: When starting feeds, especially after a period of poor intake or weight loss, your body may have trouble adjusting. Levels of important electrolytes, like potassium, phosphorus, and magnesium, can drop too low. For this reason, you often need to be in the hospital for the first few days after you start tube feedings, so your doctor can monitor and adjust these imbalances. If not corrected, these imbalances can lead to muscle weakness, heart problems, difficulty breathing, and confusion






