Lifestyle interventions
Psychological therapies
Mind-body therapies
Neuromodulation devices
Lifestyle interventions
Alcohol cessation
Back to topHow to Safely Stop Drinking Alcohol?
For patients with chronic pancreatitis, stopping alcohol consumption is essential to prevent further pancreatic damage, reduce pain episodes, and lower the risk of complications. However, alcohol cessation should be done safely, as withdrawal symptoms can be severe or even life-threatening in heavy drinkers. Before quitting, patients should speak with a healthcare provider to assess their risk for alcohol withdrawal and determine if medical supervision is needed.
Signs of alcohol withdrawal may begin within hours of the last drink and include tremors, anxiety, sweating, nausea, seizures, and in severe cases, delirium tremens (confusion, hallucinations, agitation). In such cases, detoxification with medical help is strongly recommended.
Treatment Options for Alcohol Cessation
Alcohol cessation is most successful when combining behavioral interventions and medications. Treatment should be individualized and may include:
Behavioral Interventions
- Brief counseling from a physician or psychologist.
- Cognitive behavioral therapy (CBT).
- Participation in peer-support groups (e.g., Alcoholics Anonymous).
FDA-Approved Medications for Alcohol Use Disorder
- Acamprosate: Helps maintain abstinence. Works best for patients who are already sober. Safe in liver disease but not for those with severe kidney impairment.
- Naltrexone: Reduces cravings and the pleasurable effects of alcohol. Available orally or as a monthly injection. It should be avoided in patients using opioids or with severe liver disease.
- Disulfiram: Produces unpleasant reactions if alcohol is consumed (e.g., flushing, nausea). It does not reduce cravings and works only if taken regularly as directed .
Supportive Measures
- Regular follow-ups to monitor for relapse.
- Education for patients and families about the risks of continued alcohol use and the benefits of cessation.
- Nutritional support to address deficiencies common in alcohol use and pancreatitis.
Stop drinking alcohol has long-term benefits in patients with chronic pancreatitis. Discuss with your healthcare provider the best plan to quit successfully.
Tobacco cessation
Back to topHow to Stop Smoking?
Tobacco use is associated with more pain and increases the risk of pancreatic cancer. Smoking cessation can increase the chances to improve chronic abdominal pain. The decision to quit is the first step to quit smoking, and success often improves with a structured plan and support. Strategies to quit smoking include setting a quit date, avoiding triggers, preparing for withdrawal symptoms, and seeking behavioral and medical support.
Withdrawal symptoms include irritability, cravings, anxiety, and sleep disturbances. They usually peak within a few days of quitting smoking but improve over time. These can be managed effectively with the right treatments and support.
Treatment Options for Smoking Cessation
A combination of behavioral support and medications significantly increases the chances of quitting successfully.
Behavioral Support
- Individual or group counseling.
- Telephone quit lines or mobile health apps.
- Cognitive behavioral therapy to manage triggers and habits.
- Motivational interviewing to build commitment and confidence.
First-Line Medications
- Nicotine Replacement Therapy (NRT): Available as patches, gum, lozenges, nasal spray, or inhaler. Helps reduce cravings and withdrawal symptoms by delivering low doses of nicotine without tobacco smoke.
- Bupropion: A prescription medication that reduces cravings and withdrawal symptoms. It’s also an antidepressant, which may help patients with low mood during quitting.
- Varenicline: A medication that reduces cravings and makes smoking feel less satisfying, decreasing satisfaction from smoking.
Combination Therapy
- Using more than one treatment—such as nicotine patches with lozenges or gum—may be more effective than using a single method.
Smoking cessation has long-term benefits and can slow disease progression and abdominal pain in chronic pancreatitis. Talk with your healthcare provider to make a quitting plan that works for you.
Psychological therapies
Cognitive behavioral therapy (CBT)
Back to topWhat is CBT?
CBT is a short-term, goal-directed form of talk therapy that addresses problems associated with chronic pain through changes in thinking, behavior, and feelings. This form of therapy has some of the strongest evidence supporting its use with chronic pain compared to other treatments that don’t use medicine. It can be obtained in either group or individual formats and typically lasts for 8–12 sessions, with occasional booster sessions every few months for maintenance of benefit.
How does CBT work?
CBT treatments exist for many illnesses including cardiovascular disease, diabetes, cancer, depression, anxiety and chronic pancreatitis. The commonality of these conditions is that the goal of treatment is not to fix or cure the problem but to successfully manage it over time. When used for chronic pain, CBT helps to identify thinking and behavioral patterns that may have been helpful when pain was acute (e.g., resting, avoiding people), but are now problematic given pain is chronic (e.g., prolonged rest leads to deconditioning, avoiding people interfering with work and family responsibilities).
CBT involves a patient and a therapist, each of whom has a specific role. The patient (a) identifies problems, (b) defines goals, (c) learns skills, and (d) implements solutions. The therapist (a) listens, (b) helps refine goals, (c) teaches skills, (d) reinforces/encourages trying new approaches, (e) personalizes skills for the individual for long-term use.
By changing behaviors that can make pain worse, and by altering thinking patterns that promote negative emotions, pain can diminish, and functioning can improve.
Who can be a CBT provider?
A CBT therapist is a licensed health professional with advanced training in CBT. CBT is often provided by a licensed psychologist or social worker. CBT may also be provided by nurses, physical therapists, occupational therapists or licensed professional counselors. While many providers have general CBT training, it is recommended that you identify a therapist with advanced training in CBT for chronic pain.
CBT-related self-management skills for pain without formal psychotherapy can be taught by health coaches, physician assistants and medical assistants. This is different than receiving CBT but can provide skills and practical techniques to manage chronic pain.
How to find a CBT provider?
Many Pain and some Gastroenterology Clinics will have trained CBT therapists on staff.
Alternatively, you can search for a therapist in your area using these websites:
It is worth shopping around for a therapist with whom you can relate. Much of CBT rests upon a good therapeutic relationship between the therapist and the client.
What to expect?
The first several sessions involve education and information gathering with enough time for the patient to fully tell his/her history/story of how pain started and its impact on life. The early sessions ensure that the therapist and patient share a common knowledge about how pain works within the body, agree on expectations for therapy, agree on the goals of therapy, and agree on what constitutes success/improvement.
Subsequent sessions (typically 45 minutes each) involve the therapist teaching a skill to address an issue associated with pain (e.g., sleep problems, pain intensity, negative mood, problems thinking, fatigue etc.). The skill is presented, the patient is encouraged to try the skill, and is given homework for practicing the skill between sessions. At the next session, the homework is reviewed, problems with the homework are addressed, and a new skill is introduced along with new homework. Throughout therapy, weekly monitoring of pain and function allows the patient to identify those skills that are having an impact. Near the end of treatment, the patient and therapist make a long-term maintenance plan for taking and using the most helpful skills into the future. Successful therapy is typically associated with improvements in function, decreases in pain, and confidence in using each of the skills on one's own when needed.
Potential Risks
CBT is a safe form of talk therapy for which there is minimal risk. Sometimes talking about pain can temporarily make pain seem more intense.
Acceptance and commitment therapy (ACT)
Back to topWhat is ACT?
Acceptance and commitment therapy (ACT) is a type of talk therapy that is proven to work and addresses problems associated with chronic pain by helping individuals think and act differently with respect to pain. ACT focuses on helping patients to reduce pain-related distress through increasing engagement in valued behavior. ACT provides skills that help patients learn to accept pain and focus upon improving quality of life despite pain. ACT can be performed both individually and in groups. Treatment is often short term (8–12 sessions) with follow-up as needed. ACT has strong evidence for reducing pain-related distress.
How does ACT work?
ACT focuses on the development of a rich and meaningful life despite pain. ACT interventions address universal sources of human suffering. Sometimes pain cannot be "fixed", thus ACT attempts to manage distress instead of trying to get rid of it. ACT theory is based on the notion that distress is an unavoidable component of humanity. Often, attempts to avoid distress can lead to increased suffering.
The goal of ACT is working to increase acceptance of things outside of one's control and increasing movement towards things that are valued. While the goal of ACT is not specifically to reduce chronic pain, evidence supports its efficacy for several outcomes, including increasing quality of life, decreasing distress, and decreasing mood symptoms, among other benefits. Reductions in these sources of distress often lead to patients reporting decreased pain and decreased distress related to pain. ACT may also include training in techniques which have been shown to be effective for treatment of chronic pain in other contexts, including mindfulness, relaxation, cognitive defusion, and education.
ACT involves a patient and a therapist who each have a specific role. The patient (a) identifies problems, (b) defines goals, (c) learns skills, and (d) implements solutions focusing on reducing control and increasing behavior in line with their values. The therapist (a) listens, (b) helps refine goals and clarify patient values, (c) teaches skills, frequently using metaphors and stories, (d) encourages use of new skills, and (e) provides treatment focusing on long-term use.
By accepting things that cannot be controlled (e.g. pain), the therapy focus can shift towards increasing valued behavior and quality of life. When patients have a high quality of life, pain is less influential, consequential, and patients report less pain-related distress.
What other names might this go by?
ACT is a form of psychotherapy that is typically practiced by a trained mental health professional. ACT based skills have however been implemented into a number of platforms including self-help books, websites, and support groups. ACT was developed though Relational Frame Theory, which is a term that is sometimes used in describing treatment. Training in mindfulness is a component of ACT based treatment. Multiple additional interventions utilize mindfulness but may not be related to ACT.
ACT and other forms of therapy including Cognitive Behavioral Therapy (CBT) and Emotional Awareness and Expression Therapy (EAET) may share some techniques or processes.
Who can be an ACT provider?
ACT should be provided by a licensed mental health provider, which may include a Licensed Psychologist, Social Worker, or Professional Counselor. Typically, ACT is provided by an individual who has advanced training in ACT.
The principles of ACT may also be incorporated into other forms of care, including Interdisciplinary Treatment, Physical Therapy, Occupational Therapy, Medial Treatment, and Health Coaching. These skills are often provided informally while participating in other forms of treatment.
Like other forms of mental health treatment, having a strong rapport with your ACT provider is extremely important for effective treatment. While there may be fewer ACT trained clinicians to choose from, individuals with pain are encouraged to seek a provider with whom they feel they can have a good relationship.
What to expect?
ACT treatment typically starts with a formal assessment in which the patient is asked questions related to the presenting problem, reason for seeking treatment, history, and any additional relevant information. This allows the patient to provide information about why they are seeking treatment. In the first several sessions the therapist and patient will get to know one another. Specific time will likely be spent processing the impact of pain upon the patient's life.
Early on in treatment it is likely that the topic of values will be explored, including a discussion of the impact of pain upon valued behavior. The patient and therapist will work to develop collaborative goals for treatment, typically focused on increasing function and improving quality of life. Time will also be spent working to identify what would be considered signs of progress. ACT based treatment typically focuses on improving function and increasing valued behavior versus focusing primarily on symptom reduction as measures of improvement.
In many sessions the therapist may provide education on ACT based skills. These skills will likely be presented to address a pain-related concern. ACT-based treatment is likely to focus on exploring current patterns of thinking and behavior related to pain. A fundamental goal of ACT-based treatment will be to identify and accept sources of distress that are outside of a patient's control. Patients are likely to have education in the use of mindfulness and relaxation skills. Treatment will also work to increase action toward valued behavior. Patients will be asked to attempt to implement skills discussed in treatment and are likely to receive homework from their therapist. This homework is often reviewed in session, with time spent discussing use of skills, and adapting skills as needed. In addition to specific ACT-based skills, patients are likely to receive skills for addressing other important aspects of pain such as sleep, mood, and stress management. Success in treatment is associated with improvements in function, increased confidence in the patient's ability to manage pain, increasing valued behavior, and decreased pain-related distress. ACT treatment is typically performed once a week in outpatient settings, with sessions lasting 45–55 minutes.
Potential risks
ACT is a safe form of talk therapy for which there is minimal risk. Sometimes talking about physical or emotional pain can be difficult and make pain or distress more intense for a short period of time.
Resources
Emotional awareness and expression therapy (EAET)
Back to topWhat is EAET?
Emotional Awareness and Expression Therapy (EAET) is a form of psychological therapy that targets trauma, stress, and relationship problems that are found in many people with chronic pain, especially centralized/nociplastic pain. Although all chronic pain is influenced by psychosocial factors, centralized pain conditions appear to be strongly influenced by the functions of the central nervous system, especially the brain's thoughts, feelings, and relationships. Such pain conditions include cases of chronic pancreatitis, fibromyalgia, irritable bowel syndrome, head pain, and many cases of back or other localized pain. Research shows that stress throughout people's lives and how they handle the emotions from that stress, can trigger, worsen, or maintain their pain. Most psychological treatments for these pain conditions, including traditional Cognitive Behavioral Therapy (CBT) and Acceptance and Commitment Therapy (ACT), do not focus on helping people resolve these earlier life stressors, but this is the focus of EAET. This form of therapy is rather new, and so only a handful of clinical trials have been published testing it. Many case reports suggest that EAET can be quite powerful, even leading to the remission of pain in some people.
How does EAET work?
EAET can be conducted in individual or group sessions, and studies thus far have tested EAET protocols that range from a single, 90-minute session to 8 group sessions. It is likely, however, that more sessions are needed for many patients, because this therapy tries to address problems that are often long-standing in people's lives. Unlike CBT, which seeks to help people manage their pain and improve their adjustment to a chronic condition, EAET views centralized pain as potentially reversible if the person makes powerful changes in their emotions and relationships. EAET involves four components. First, patients are educated about the role of stress and emotions in their pain by using examples from their lives and demonstrations during intensive interviews. Second, patients are helped to disclose and talk or write about the traumas and psychological conflicts in their lives that appear to drive their pain. Third, patients are helped to express the emotions that they have been avoiding or blocking related to trauma or stressors, especially their anger but sometimes also their sadness, guilt, love, and self-compassion. Finally, given the newfound awareness of their feelings, patients learn how to communicate more effectively in real relationships by balancing assertiveness and healthy boundaries with openness and closeness. When patients are able to make these changes, they commonly have substantial pain reduction and their mood, physical functioning, and relationships will also improve.
What other names might this go by?
EAET borrows from other therapies that help people resolve trauma and psychological conflicts, including Prolong Exposure Therapy, Intensive Short-term Dynamic Therapy (ISTDP), Emotion-focused Therapy, Written Emotional Disclosure, and Rescripting Therapy. A common process of all of these therapies is that they offer support in helping patients face their traumas and conflicts, become aware of their feelings, experience their emotions, and express them in adaptive ways. These therapies, as well as others designed for trauma (e.g., Eye Movement Desensitization and Reprocessing and Cognitive Processing Therapy), are supported by research as being helpful to people who have post-traumatic stress disorder, and recent research supports many of these treatments for people who have chronic pain and trauma symptoms.
Who can be an EAET provider?
Because EAET is rather new, there are few providers who have been trained specifically to deliver it. However, many psychologists and other mental health providers have training in trauma-focused therapies and "exposure-based" therapies that help patients overcome their fears. Such therapists may be able to provide EAET-like interventions for patients, especially when patients openly discuss with these therapists that working on their avoided emotions and troubled relationships is what is needed.
What to expect?
The first several sessions usually involve learning about patients' health and psychosocial history, including stresses or traumas that have been experienced. The therapist will help patients see links between their pain and their emotional life experiences. Therapy has patients revisit important conflicts or traumatic experiences that involve other people and helps patients "express the unexpressed" feelings to those people. This can be done with writing exercises but also involves "talking to" an empty chair where the imagined other person sits. Patients are encouraged to activate and express their emotions fully, using their words, voice tone, and bodily expression (arms, face). Patients are helped to express the full range of avoided emotions, including anger, sadness, love, guilt, and self-compassion. Relief and some reduction in pain is usually felt after doing such exercises, but patients often need to do this "experience and expression" work several times. Finally, patients are encouraged to plan and role play how they would like to be in real life with people who have been a source of stress or conflict. Such communication depends on the type of relationship and may involve healthy assertiveness and setting boundaries, and often includes being open, vulnerable, and expressing intimacy. Throughout therapy, patients are encouraged to work on emotional awareness, writing exercises, emotional expression, and healthy communication as homework. Successful EAET is typically associated with reduction in pain as well as improvements in functioning, mood, and relationships.
Potential Risks
EAET and related approaches are associated with greater risk than CBT and ACT and other psychological treatments for chronic pain. EAET encourages patients to disclose and emotionally express experiences and feelings that may have been avoided for many years and that often are quite upsetting. It is not uncommon, therefore, for patients to become temporarily more upset (e.g., anxious, depressed, angry) as they start to deal with memories and feelings that have long been avoided. Pain and other physical symptoms sometimes increase temporarily. Because patients are encouraged to communicate and interact differently in their relationships, these relationships might change in ways that are unexpected. Practitioners of EAET believe, however, that such emotional and relationship changes are important to make, and even though they may be difficult in the short run, such changes can be healthy and lead to pain reductions in the longer-term. EAET, however, may not be appropriate for certain patients, especially those who have difficulties regulating their emotions, who dissociate or have trouble thinking when they are emotional, or who tend to hurt themselves or others when memories or feelings are activated or intense.
Resources
- Psychophysiologic Disorders Association
- Tension Myositis Syndrome Wiki (TMS Wiki), including its link to Alan Gordon's Pain Recovery Program
- Unlearn Your Pain (3rd Edition) by Howard Schubiner
Mind-body therapies
Acupuncture
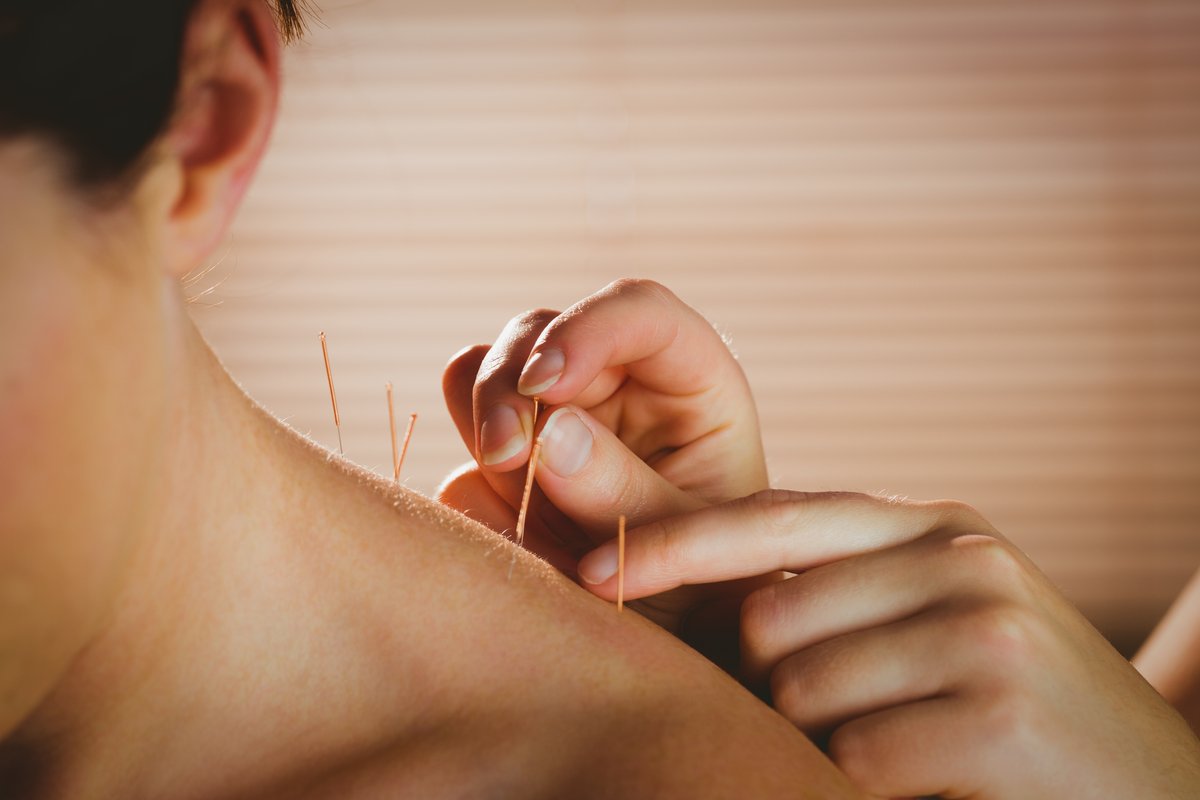
Back to topWhat is acupuncture?
Acupuncture is a component of Traditional East Asian Medicine (TEAM). It has been used as a medical intervention for over 4,000 years. The earliest records of acupuncture can be traced to the use of Bian Stones in China. These stones are believed to be used in applying pressure to specific spots on the body to promote health. Today acupuncturists use sterile thin needles that are inserted into the body to stimulate points called acupoints, along energy channels or meridians. These pathways run along the body where chi or energy flows. By stimulating the acupoints, various illnesses and symptoms can be treated. Once the needles are inserted, the acupuncturist may stimulate them in a number of different ways. This can be either manually with a rotation or thrusting motion, electrically with a stimulation device, or thermally with an herb called moxa that burns similarly to incense. The needles are usually retained in the body for 15–30 minutes and then removed. Needling elicits a dull achy sensation, warmth, or even an electrical propagation within the body. This is called the De Qi sensation and while not uncomfortable, it is often described as a unique sensation that most Westerners have not experienced before. Following needle removal there may be a drop or two of blood but typically the process does not cause bleeding. Different acupoints are stimulated depending on what symptoms are being treated. Acupuncture can also be personalized to match unique symptoms and characteristics of the person being treated.
How does acupuncture work?
While acupuncture has been practiced for thousands of years, Western scientists have only studied the effects of acupuncture on animals and humans since the mid-1960s. While acupuncture has been employed historically to treat numerous medical conditions, most investigations have shown it to be useful for reducing chronic pain, decreasing anxiety, improving sleep, and reducing fatigue. There is evidence showing that acupuncture can reduce pain from chronic pancreatitis.
While we currently don't know how inserting acupuncture needles into specific acupoints on the body helps improve symptoms such as chronic pain, the effects are different from a simple placebo. Strong evidence supports the notion that acupuncture elicits changes in the nervous system and brain. These effects include changing the levels of chemical messengers, called neurotransmitters, which when too high or too low can be responsible for causing symptoms such as chronic pain. Acupuncture also appears to modulate cell activity in the muscles and skin, regulating certain signaling molecules. Work in the field of blood pressure has shown that not all acupoints cause the same effects in the body. Instead, specific acupuncture points appear to have unique functions that are specific to that point. The ways in which acupuncture works likely depend upon which points are being stimulated.
From a Traditional East Asian Medicine (TEAM) perspective, acupuncture needling simply regulates the flow of chi or energy within the body. This chi or energy is thought to flow along channels or meridians, and this can be thought of much like the motion of water in a river. If the river is either too dry or overflowing, the surrounding land can suffer. Similarly, energy flow along meridians in the body can either be deficient or in excess. Based on TEAM theory, this can lead to illness. The flow of chi or energy along the meridians can either be turned up, in cases where there is a deficiency, or reduced if there is an excess, in order to balance the flow of chi. The acupuncturist does this by inserting needles at specific acupuncture points.
How to get started with acupuncture?
Acupuncture should be provided by a licensed or registered healthcare provider. This may include a Licensed Physician or Nurse, or a Professional Licensed Acupuncturist depending on which state in the US that you live in. This individual should have advanced training in acupuncture. The main credentialing organization for Traditional East Asian Medicine in the United States is the National Certification Commission for Acupuncture and Oriental Medicine. Their website is: https://www.nccaom.org/
On this site, you can find a registered acupuncturist in your area using the following link: https://www.nccaom.org/find-a-practitioner-directory/
Like other forms of healthcare treatment, having a strong rapport with your acupuncturist is important. In choosing your acupuncturist you may want to consider the following:
-
Find a practitioner that takes your medical insurance. Acupuncture has been approved by Medicare and Medicaid for the treatment of low back pain. However, not all acupuncturists take insurance.
-
You may need to travel to your acupuncturist for multiple sessions. For chronic conditions, one treatment session may not be enough, and you may need multiple sessions to manage your symptoms.
-
You may want to wear comfortable clothes so that the acupuncturist has access to your acupoints.
-
Needling of the acupoints may feel warm, tingly or even achy, but it should not feel like a sharp pain.
-
Do not stop in the middle of a treatment plan; it is important to attend all of your sessions.
What to expect?
Sometime during the course of your treatments, you may experience improvement in your main symptom. You may also find improvement in other symptoms as well. This is because Traditional East Asian Medicine is designed to treat you as a whole person, not just the part of your body where you have your main complaint such as pain. After you complete your initial treatment sessions, you may be able to stop doing acupuncture and maintain good pain control as well as stable reductions in your other issues. If your symptoms worsen, feel free to go back to doing acupuncture and also consider doing self-acupressure as a safe, easy to learn intervention that works similar to acupuncture but does not use needles. Different people have different reactions to these treatments – find what works for you.
Potential risks
Acupuncture is generally considered very safe. Occasionally people can experience bruising at acupoint sites or slight bleeding. If bruising or bleeding occur, consider taking a few days off from doing acupuncture or ask the clinician not to insert needles where there is bruising or where bleeding may occur. If bruising or bleeding persist, stop doing the acupuncture, it may not be right for you.
Yoga
Back to topWhat is yoga?
Yoga is an ancient set of practices that originated in India. These practices include a rich philosophical tradition, an ethical and moral framework, physical postures (called asanas), breathing techniques (pranayama), and meditation. There are many different yoga traditions and schools which draw on various aspects of these practices. For example, many yoga teachers in the United States focus solely on breath and postures. Yoga is often taught in individual or group classes.
How does yoga work?
While yoga has been practiced for thousands of years, Western scientists only started doing yoga studies over the past several decades. Yoga has been employed historically to treat numerous medical conditions, and recent studies have shown that yoga can be a useful chronic pain management strategy by reducing stress and anxiety, decreasing pain, and enhancing strength and flexibility. There is data that 1-hour of yoga sessions 3 times a week can improve the quality of life in patients with chronic pancreatitis. The ways in which yoga works likely depend on which yogic practices are employed, as there is much overlap between the benefits of yoga practices and other mind-body techniques (e.g. meditation).
Yoga postures can help strengthen or stretch parts of the body that are weak or stiff, as well as enhancing bodily awareness and pain tolerance. Breathing practices can improve lung function, increase relaxation, and help practitioners improve emotional regulation. Meditative practices can enhance focus, concentration, and mental/emotional clarity, while also supporting bodily, mental, and emotional awareness. Taken together, these practices can help practitioners identify behaviors and thoughts that contribute to worsened pain, as well as teaching movements and skills to help accept or lessen pain.
Unfortunately, because of the lack of standardization in teaching, unreliable insurance coverage, and the relatively new state of the medical literature, the burden of finding the right yoga teacher and practice(s) fall upon patients and their practitioners.
What are some common yoga styles?
- Hatha: Generic term referring to yoga classes that include physical postures. Typically involves slower movement and holding poses for longer.
- Vinyasa: More dynamic movement, links breath to movement, variable sequencing, lively music.
- Ashtanga: Very physically rigorous, links breath to movement, same order of sequences in every class.
- Restorative: Gentle movements, lots of supports (e.g., blocks, blankets), long holds in each posture.
- Hot yoga: Same order of sequences in every class, artificially heated classrooms that are 95º Fahrenheit or warmer.
Who teaches yoga?
In the US, yoga is typically taught by certified yoga teachers. These teachers may have variable degrees of training (200, 500, or 1000 hours) as well as specialty certifications, such as prenatal, children's, or trauma-sensitive yoga. There are many yoga and teaching styles, so it is worth searching for a teacher whose style aligns with your specific needs or preferences.
While not always appropriate for someone who is completely new to yoga, there are numerous free online yoga videos that are available (see Resources).
Note: Most yoga classes are not covered by insurance. This may differ depending on where you live.
What to expect?
As there are many different schools of yoga and yoga styles, what to expect will vary in each class. Most classes are 60 to 75 minutes long, have multiple participants (5–20), and are mat-based. Classes typically cost $10–$30. An example of a typical one-hour class is as follows:
- Centering (5–10 minutes): Using breathing exercises or a gentle warm up to try to become more present in the space and the body. This is also the time during which the intention for the class is set.
- Movement (40–50 minutes): The sequence of postures will vary depending on which part(s) of the body are being targeted and the relative physical rigor of the class.
- Rest and relaxation (5–10 minutes): Lying down, resting, and/or meditation.
Depending on the yoga teacher and style of yoga, the class may also involve chanting, longer periods of meditation or breathing exercises, and checking-in with the teacher before or after class. If you are unsure of or are uncomfortable with certain practices, it is important to check-in with the teacher or studio owner to ensure that you choose a class in alignment with your needs.
It is also possible to schedule private yoga lessons, which often cost $50–$120 per hour. These lessons involve more personalized instruction and may represent a useful way to build the foundation of a yoga practice if you are unfamiliar with yoga and/or are uncomfortable participating in a large class.
Potential Risks
Yoga is generally considered quite safe. As with other forms of exercise, it is possible to overexert oneself, fall down, or endure other injuries. It is important to pay attention to the body to ensure that the movements align with individual needs. Consider starting with low impact, gentle classes and gradually increasing intensity if desired.
Resources
- You can find a school or yoga teacher registered through the Yoga Alliance.
- You can practice yoga with free online videos. One such resource is Yoga with Adriene.
- You can also practice yoga through subscription sites, such as Jamie Elmer's.
Neuromodulation devices
A neuromodulation device is a medical device that delivers electrical impulses to nerves or the spinal cord to help reduce chronic pain. These devices have been effective in treating certain pain conditions like back pain or neuropathy, pain arising from nerves. However, their use for chronic pancreatitis pain is still considered experimental, as there is limited evidence to support their effectiveness in this condition.
Transcutaneous electrical nerve stimulation (TENS)
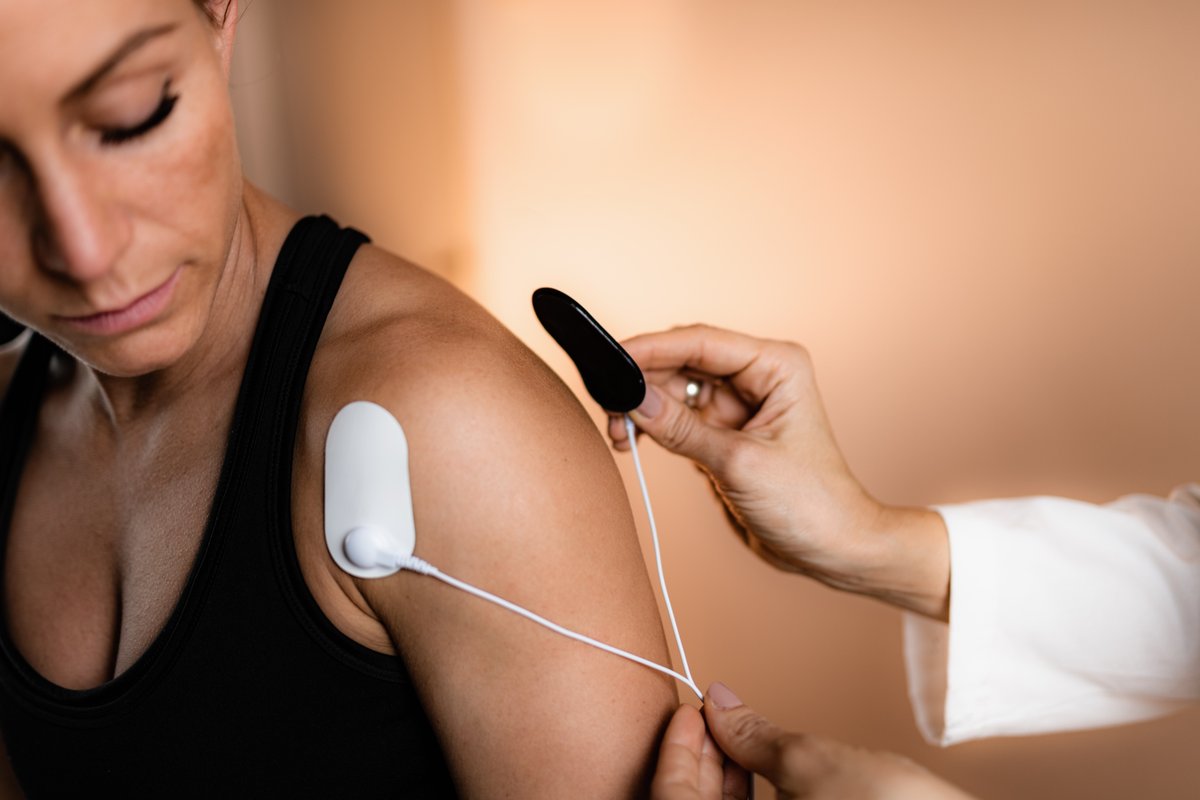
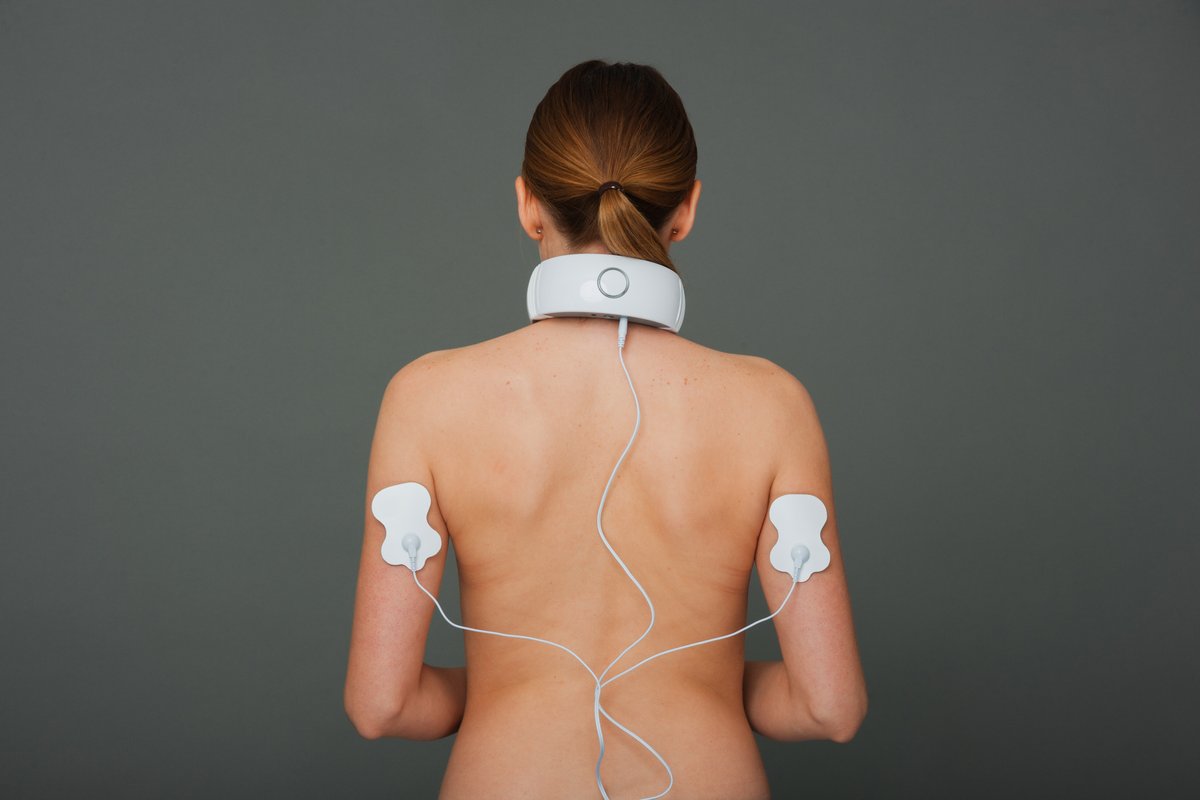
Back to topHow does TENS work?
TENS works through the delivery of small electrical impulses. These impulses start in the TENS unit (a small hand held machine), travel down electrodes, and into pads on the skin. These treatments are self-applied by patients based on doctor's instructions. The pads are specially designed to deliver the electrical impulse into the tissues and nervous system of the patient's body. The nervous system picks up on these electrical impulses and sends signals to the brain which masks the sensation of pain from that area.
What to expect?
When chronic pain is local and specific, the use of an electrical stimulator can be effective to dull the pain temporarily. Typically, this kind of modality is used after the intervention has proven to be helpful in the clinic, and is only used by the individual during very specific activities. You can expect to feel a strong tingling sensation under the pad which is attached to the skin. When successful, this tingling over-rides the pain sensations, and provides relief. The body is able to build a resistance to this TENS, so the longer it is used, the less effective it becomes.
Potential Risks
Patients with pacemakers should avoid this equipment because the electrical current could interfere with the pacemaker. There is a low occurrence of burns when the electrodes are not placed correctly, or the power is turned up too high.
Spinal cord stimulation (SCS)
Back to topWhat is the purpose of this procedure?
Spinal cord stimulation (SCS) is an implantable pain relief therapy. The surgeon implants a device into the body that sends a low electric current to your spinal cord to block pain signals traveling to your brain. SCS has been FDA approved to relieve chronic pain from nerve damage in the trunk, arms, or legs since 1989. The most common situations it is used for are failed back surgery, complex regional pain syndrome, and peripheral neuropathic pain caused by nerve damage beyond the spine or brain. The permanent device used in the therapy is similar in appearance to a pacemaker. It consists of an impulse generator, battery and leads to carry the electrical signal to the target nerves. When considering if SCS may be helpful for you, it is important to have a thorough assessment with your doctor. Following this a test period called a "trial" is arranged. During the trial a temporary device is used to give you an idea of what it would be like to have a stimulator. Trials typically last seven days. At the end of the trial the temporary leads are removed. If the trial is successful, a permanent system can be implanted through small cuts or incisions.
What will happen during the procedure?
The procedure is performed on an outpatient basis in a special procedure room equipped with a fluoroscope (x-ray). In the pre-procedure area, the nurse or doctor will place an IV line. This is used for fluids and sedation.
When you get to the procedure room for your safety and comfort you will be connected to monitoring equipment (EKG monitor, blood pressure cuff, and blood oxygen monitoring device) and positioned on your stomach.
Your back is cleansed with an antiseptic soap after which the doctor injects numbing medicine into your skin. This will cause a burning sensation for a few seconds.
The doctor then carefully directs a needle with help of the fluoroscope (x-ray) to the epidural space. Once positioned correctly, a thin lead is passed through the needle. The lead is advanced until the small contacts on the end of the needle are over the target location.
The leads are connected to the impulse generator then turned on. You will feel a tingling sensation called a paresthesia. The device representative will ask you several questions such as where you feel it and how strong it is.
When the device is in the correct location it will be secured in place.
Potential risks
The risks are infrequent. They include:
- Allergic reaction to medication
- Nerve damage (spinal cord and nerve roots)
- Bleeding and bruising at the injection site
- Pain at the injection site or during the procedure
- Infection
- Puncture of the sac surrounding the spinal cord (dura mater)
- Spinal headache
- No improvement or worsening of your pain in some cases
A common complication is movement of the leads during the trial. This is called lead migration. If the leads move during the trial your painful areas may not be covered. This makes it hard to determine whether or not it would work for you.
Non-invasive vagal nerve stimulation (nVNS)
Back to topWhat is non-invasive vagal nerve stimulation (nVNS)?
nVNS is a technique that uses electrical impulses to stimulate the vagus nerve and treat chronic pain without the need for surgical implantation. A device with an electrode is placed on the skin, usually on the neck or ear, to deliver mild electrical pulses to the vagus nerve.
How does VNS work?
nVNS works by stimulating the vagus nerve, which plays a key role in regulating pain pathways in the brain. The electrical stimulation activates the pain control system in the brainstem, which reduces pain perception.
What to expect?
During a session, you will place the device on your skin, typically on the neck or ear, where it delivers electrical pulses. You may feel a tingling or mild discomfort in the area during the stimulation. Sessions usually last 15-30 minutes and can be done multiple times a day from home. Some people notice improvements in pain or symptoms after a single session, though the effects may take longer to be significant.
Potential risks
nVNS is generally safe, but there are some risks. You may experience skin irritation or discomfort at the site where the device is applied. Some users report headaches or a feeling of lightheadedness during or after stimulation. It is contraindicated for people with pacemakers, implantable defibrillators, or other electrical implants, as it may interfere with the device.
Repetitive transcranial magnetic stimulation (rTMS)
Back to topWhat is Repetitive Transcranial Magnetic Stimulation (rTMS)?
rTMS is a non-invasive procedure that uses magnetic fields to stimulate specific areas of the brain. It is primarily used for treating neurological and psychiatric conditions such as depression, chronic pain, and migraines.
How does rTMS work?
rTMS works by using magnetic pulses to stimulate neurons in the brain, which can change brain activity and influence the brain's pain modulation pathways. These pulses help suppress pain signals.
What to expect?
During an rTMS session, a coil is placed on your scalp near the targeted brain area. The device delivers magnetic pulses, which you may feel as a tapping sensation on your scalp. Each session typically lasts 20-40 minutes, and treatments are usually done daily or a few times a week for several weeks. You may experience temporary discomfort like headache or scalp twitching, but it is generally well tolerated. This is only done at a doctor's office or research facility.
Potential risks
rTMS is generally safe, but some risks include mild headache, scalp discomfort, or lightheadedness during or after treatment. Rare side effects include seizures, especially for individuals with a history of epilepsy. It is contraindicated for patients with implanted metal objects in their head or neck area, like pacemakers or stents, as it may interfere with these devices.